The Invisible Assault on Our Health
By Dr Jack Austin Warner
Part II
In Part I, we argued that Saharan dust is no longer a seasonal curiosity but a climate-linked public health challenge. In Part II, we must confront the harder truth: this haze is not simply uncomfortable. It can be deadly.
When Saharan dust blankets the Caribbean, what we see is only part of the threat. The real danger lies in the microscopic particles suspended in that grey sky; particularly what scientists call PM2.5. These are particles measuring 2.5 micrometres or smaller, about thirty times thinner than a human hair. Their size is precisely what makes them dangerous.
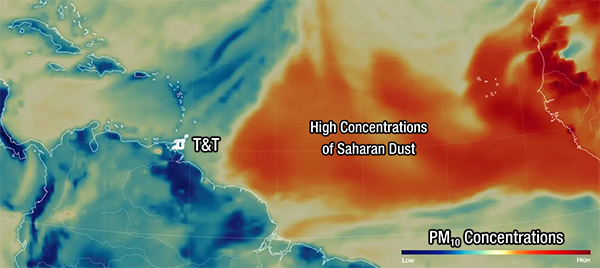
It is important to clarify something. Saharan dust contains a range of particle sizes. Some particles are larger, closer to PM10, and irritate the eyes, nose, and throat. But within these dust plumes are also fine and ultra-fine particles that fall within the PM2.5 range.
These smaller particles can penetrate deep into the lungs and even enter the bloodstream. When we talk about the most serious health consequences of Saharan dust, PM2.5 is central to the discussion.

A thick blanket of Saharan dust covers Port-of-Spain
Unlike visible dust that gets trapped in the upper airways, PM2.5 bypasses many of the body’s natural defences. It travels down into the alveoli, the tiny air sacs responsible for oxygen exchange. From there, particles can pass into the circulatory system, triggering inflammation not just in the lungs but throughout the body.
The illnesses associated with heavy dust exposure are not hypothetical. Hospitals across the region routinely report spikes in asthma attacks during intense dust episodes. Children with pre-existing respiratory conditions struggle to breathe.
Elderly citizens experience worsened chronic obstructive pulmonary disease (COPD). Sinus infections, bronchitis, persistent coughing, chest tightness, and throat irritation increase sharply, but the respiratory system is only the beginning.
From the landmark Harvard Six Cities cohort (Dockery, Pope) to major cohort analyses (Pope) and consensus clinical statements (Brook et al., AHA; Newby et al., ESC), the evidence consistently links PM2.5 exposure to cardiovascular inflammation and increased risk of heart attacks, strokes, arrhythmias, heart failure, and cardiovascular mortality.
For individuals with underlying heart disease, even short-term exposure can be dangerous. In severe cases, particulate pollution has been associated with premature mortality.

There are additional concerns unique to Saharan dust. Studies have found that these plumes can carry not only mineral particles but also microbial life: fungal spores, bacteria, and other biological materials transported across the Atlantic. While much remains under study, this raises further questions about long-term exposure and immune system stress.
Outdoor workers are particularly vulnerable
The Caribbean’s climate compounds the impact. High humidity can trap particulates close to ground level. Heat stress increases physiological strain. Urban pollution from vehicles and industrial sources mixes with dust, amplifying overall air toxicity. In densely populated communities, exposure is constant and inescapable.
Outdoor workers are particularly vulnerable. Construction workers, vendors, agricultural labourers, and delivery drivers inhale these particles for hours at a time. Children walking to school, elderly citizens without air-conditioned homes, and individuals living in poorly ventilated housing face prolonged exposure. For them, Saharan dust is not an occasional inconvenience; it is a recurring health burden, and yet, our policy responses remain fragmented.

San Fernando was not spared from the thick Sahara Dust
We do not treat dust events with the urgency applied to hurricanes, even though they occur far more frequently. Air quality monitoring remains inconsistent across islands. Public advisories are sometimes delayed or vague. Protective guidance is not systematically integrated into school or workplace protocols.
If PM2.5 levels were rising from an industrial accident, there would be outrage. When it arrives on the wind, we shrug. That must change.
Continuous air quality surveillance should be standard across the region, with real-time public reporting. Clear health thresholds should trigger mandatory advisories, especially for schools and outdoor labour sectors. Healthcare systems should anticipate seasonal respiratory surges and allocate resources accordingly.
Public education must move beyond awareness and into behavioural adaptation, limiting outdoor activity during peak events and using appropriate protective masks such as the N95, KN95, and KF94, especially to safeguard vulnerable populations. Do not use cloth masks that do not reduce particulates.
The sky turning grey is not merely an atmospheric event. It is a warning signal of systemic vulnerability in an era of climate change. Saharan dust may originate thousands of miles away, but its consequences settle in our lungs, our bloodstreams, and our hospitals.
If we fail to adapt, the cost will not be measured only in haze; it will be measured in health outcomes, and that is a price the Caribbean cannot afford to ignore.